Integrating predictive models into healthcare workflows is crucial for transforming analytical insights into actionable clinical outcomes.
Predictive models built using machine learning, statistical forecasting, and real-time data analysis help identify patient risks, predict disease progression, optimize resource allocation, and support early intervention decisions.
However, the true value of these models is realized only when they are seamlessly embedded into everyday clinical processes such as patient triage, diagnostic evaluation, treatment planning, hospital operations, and chronic disease management.
The integration process involves aligning model insights with clinician workflows, ensuring interoperability with EHR systems, maintaining data quality, and designing interfaces that present predictions in a clear, usable format.
Models must not only deliver accurate predictions but must also be explainable, timely, and clinically relevant.
Implementation requires collaboration between clinicians, data scientists, IT teams, and administrators to ensure that the model outputs support decision-making without overwhelming users or disrupting critical care processes.
With advancements in automation, real-time analytics, cloud deployment, and AI-driven decision support systems, predictive models are increasingly being used to reduce patient readmissions, detect deteriorating conditions, optimize hospital staffing, and personalize treatments.
When effectively integrated, these models enhance clinical efficiency, reduce errors, improve outcomes, and support a proactive approach to patient care rather than a reactive one.
Implementation Framework for Predictive Healthcare Models
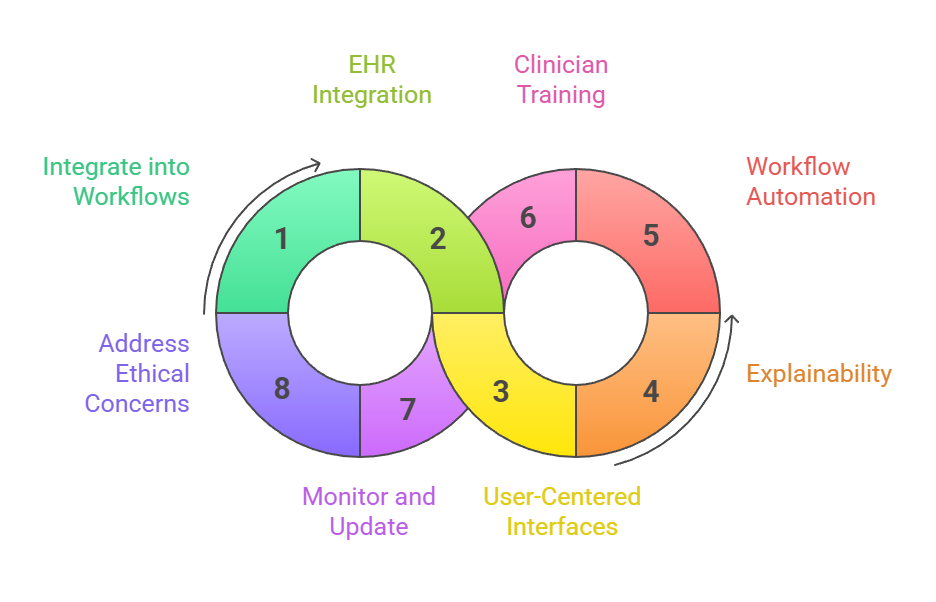 1. Importance of Seamless Integration into Clinical Workflows
1. Importance of Seamless Integration into Clinical Workflows
Predictive models must fit naturally into the clinician’s workflow to ensure adoption and effectiveness.
If predictions are difficult to access, too technical, or poorly timed, clinicians are unlikely to use them.
Seamless integration ensures that insights appear at the point of care during chart review, triage, medication prescribing, or discharge planning allowing decisions to be informed instantly.
This alignment minimizes friction and prevents workflow disruptions. It also improves trust because clinicians see immediate relevance to their tasks.
Ultimately, seamless integration increases usability, reduces cognitive load, and ensures that predictive analytics delivers real clinical impact.
2. EHR Integration and Interoperability Requirements
For predictive models to function effectively, they must be deeply integrated with Electronic Health Record (EHR) systems.
EHR integration allows models to access up-to-date patient data and provide predictions automatically, without manual inputs.
Interoperability standards such as FHIR and HL7 enable consistent data exchange across systems, making integration smoother.
When models operate within the EHR interface, clinicians can see risk scores, alerts, and recommendations within familiar screens. This reduces disruption and promotes ease of adoption.
Effective interoperability ensures scalability, prevents data silos, and supports unified patient care across departments and facilities.
3. Presenting Predictions Through User-Centered Interfaces
The design of interfaces is crucial for delivering predictions that are easy to interpret and actionable. User-centered interfaces focus on clarity, simplicity, and minimal cognitive burden.
Visualizations such as risk meters, trend graphs, and color-coded alerts help clinicians quickly understand model outputs.
Explanations that show “why” a prediction was made increase transparency and reduce skepticism. Interfaces must avoid alert fatigue by showing only relevant and high-priority warnings.
Well-designed interfaces support faster decision-making and improve clinician satisfaction with predictive tools.
4. Ensuring Explainability and Clinical Interpretability
Predictive models must be interpretable enough for clinicians to understand the reasoning behind their outputs.
Techniques such as SHAP values, feature importance, and interpretable model dashboards help explain the key factors influencing predictions.
Clinicians rely on these explanations to justify decisions, especially in high-risk scenarios like ICU care or cancer diagnosis.
Lack of transparency can lead to mistrust and low adoption rates, even if the model is highly accurate.
Explainability also supports regulatory compliance, ethical oversight, and validation of model performance. Transparent predictions help clinicians use model insights responsibly.
5. Workflow Automation and Trigger-Based Predictions
Workflow automation ensures that predictions are generated and delivered at precisely the right time.
Trigger-based mechanisms activate models when specific conditions are met such as new lab results, vital sign changes, or a completed patient assessment.
Automation eliminates manual steps and ensures real-time insights, which is critical for detecting early deterioration or preventing adverse events.
Automated alerts help clinicians prioritize high-risk patients and allocate resources effectively. This proactive approach supports faster interventions and reduces preventable complications.
Workflow automation enhances the overall reliability and efficiency of predictive model deployment.
6. Training Clinicians and Encouraging Model Adoption
Successful integration requires that clinicians trust and understand the predictive tools being introduced.
Comprehensive training sessions demonstrate how the models work, how predictions should be interpreted, and how they fit into clinical pathways. Continuous feedback loops help refine models based on clinician experience.
Addressing concerns about accuracy, false alarms, and usability increases adoption.
When clinicians feel confident using predictive insights, they incorporate them more consistently into decision-making.
Training promotes long-term engagement and ensures models remain relevant, ethical, and aligned with clinical needs.
7. Monitoring, Evaluation, and Continuous Model Updating
Predictive models must be monitored regularly to detect performance drift, bias, or deteriorating accuracy over time.
Changes in patient populations, clinical practices, or hospital data may reduce model reliability.
Continuous evaluation ensures that the model remains valid and trustworthy.
Updating the model with new data, recalibrating thresholds, and integrating new features prevents degradation.
Monitoring also ensures compliance with safety standards and regulatory requirements.
8. Addressing Ethical, Legal, and Safety Considerations
Integration of predictive models must consider patient privacy, algorithmic fairness, and the potential risks associated with incorrect predictions.
Ensuring that the model does not reinforce biases or produce harmful disparities is a core requirement.
Legal frameworks such as HIPAA, GDPR, and emerging AI regulations guide the safe use of predictive analytics.
Validating models across diverse patient populations reduces risks and enhances fairness.
Ethical integration promotes responsible AI use and ensures that predictive insights contribute positively to patient outcomes and clinical safety.
