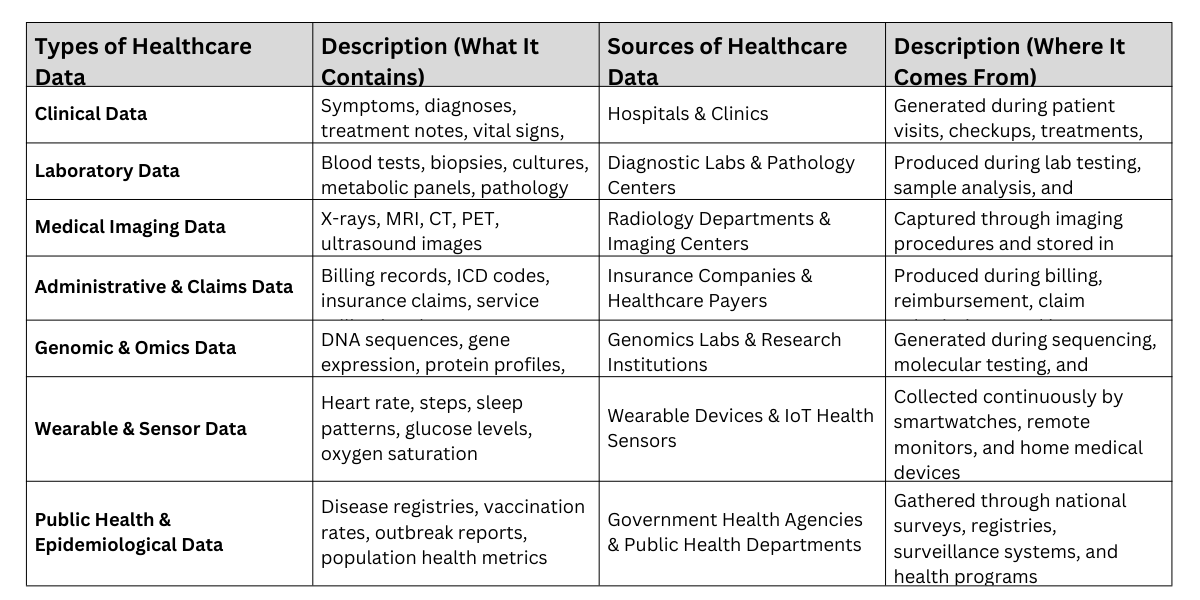
Types and sources of healthcare data refer to the various kinds of information generated, collected, and used across healthcare systems for clinical care, research, and decision-making.
This data comes from multiple origins, including patients, healthcare providers, medical devices, and administrative systems.
Understanding these data types and their sources is essential for effective data analysis, interoperability, and the development of data-driven healthcare solutions.
TYPES OF HEALTHCARE DATA
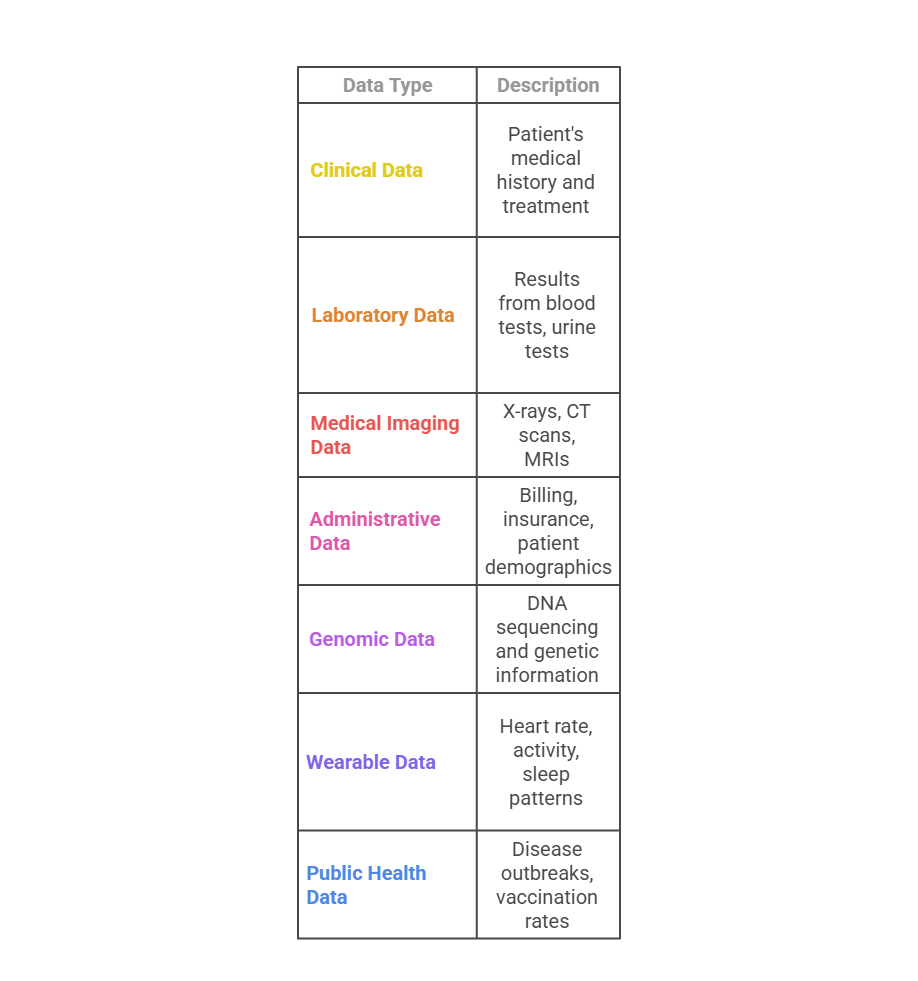 1. Clinical Data
1. Clinical Data
Clinical data includes patient symptoms, diagnoses, treatment notes, vital signs, physical exams, and clinical observations recorded during healthcare encounters. It forms the core of medical decision-making and reflects real-time patient health status.
This data can be structured like lab readings or unstructured, such as doctor notes and discharge summaries. Clinical data helps identify disease patterns, track treatment effectiveness, and monitor patient recovery.
It is essential for developing clinical decision support systems and predictive health models. As it directly captures patient health interactions, it remains one of the most reliable data types in healthcare analytics.
2. Laboratory Data
Laboratory data consists of test results from blood tests, biopsies, microbiology exams, metabolic panels, and genetic screenings. It is highly structured, numeric, and scientifically validated, making it extremely useful for data modeling.
Lab results help clinicians confirm diagnoses, detect abnormalities, and monitor disease progression.
They provide objective measurements such as blood glucose levels, hormone counts, cholesterol values, and organ function markers. Laboratory data ensures precise clinical evaluation and supports early warning systems for critical conditions.
Its accuracy and standardization make it a foundational component of healthcare data science.
3. Medical Imaging Data
This includes X-rays, CT scans, MRIs, PET scans, mammograms, and ultrasound images. Imaging data provides visual insights into internal organs, tissues, bones, and tumors, making it crucial for diagnostics.
These data files are extremely large and complex, requiring specialized software and interpretation by radiologists.
With modern AI, deep learning models analyze imaging data for early detection of cancer, fractures, organ abnormalities, and neurological conditions.
Imaging data supports treatment planning, follow-up evaluations, and surgical decisions. Its combination of visual and anatomical detail makes it indispensable in precision medicine.
4. Administrative and Claims Data
Administrative data covers billing records, insurance claims, procedure codes, diagnosis codes, and healthcare service usage. This type of data helps understand the financial and operational aspects of healthcare.
]Claims data reveals patterns of service utilization, cost distribution, reimbursement trends, and potential fraud. It is widely used in health economics, hospital management, and policy planning.
Although not clinically detailed, administrative data covers large patient populations and long historical periods. This makes it essential for big-data analysis and population-level insights.
5. Genomic and Omics Data
Genomic, proteomic, and metabolomic data capture information about genes, proteins, metabolites, and molecular pathways. These data types support personalized medicine by revealing genetic risk factors, treatment responses, and inherited conditions.
They are extremely high-dimensional and require powerful computational tools for interpretation.
Genomic data helps identify biomarkers for cancer, autoimmune diseases, and rare disorders.
It also guides targeted therapies that match a patient’s DNA profile. As genomic sequencing becomes more affordable, this data type is transforming healthcare research and individualized care.
6. Wearable and Sensor Data
Wearables generate continuous, real-time data on heart rate, sleep cycles, oxygen saturation, activity levels, glucose levels, and stress patterns.
These devices include smartwatches, fitness trackers, ECG patches, home BP monitors, and remote health sensors. Such data enables early detection of anomalies and supports chronic disease monitoring outside hospital settings.
Wearable data provides long-term behavioral insights that enrich traditional clinical datasets.
It enhances preventive care by identifying early risk signals for heart disease, diabetes, or sleep disorders. For data science, this time-series data allows advanced modeling and personalized health predictions.
7. Public Health and Epidemiological Data
Public health data includes disease registries, vaccination databases, outbreak surveillance, environmental health metrics, and demographic health statistics. It helps track disease trends, assess health risks, and plan public health interventions.
This data type is essential for epidemic forecasting, resource allocation, and policymaking. Public health datasets reveal disparities across regions and populations, enabling targeted health programs.
They support long-term monitoring of chronic diseases such as cancer, diabetes, and cardiovascular conditions. For data scientists, these datasets are crucial for population-level modeling.
SOURCES OF HEALTHCARE DATA
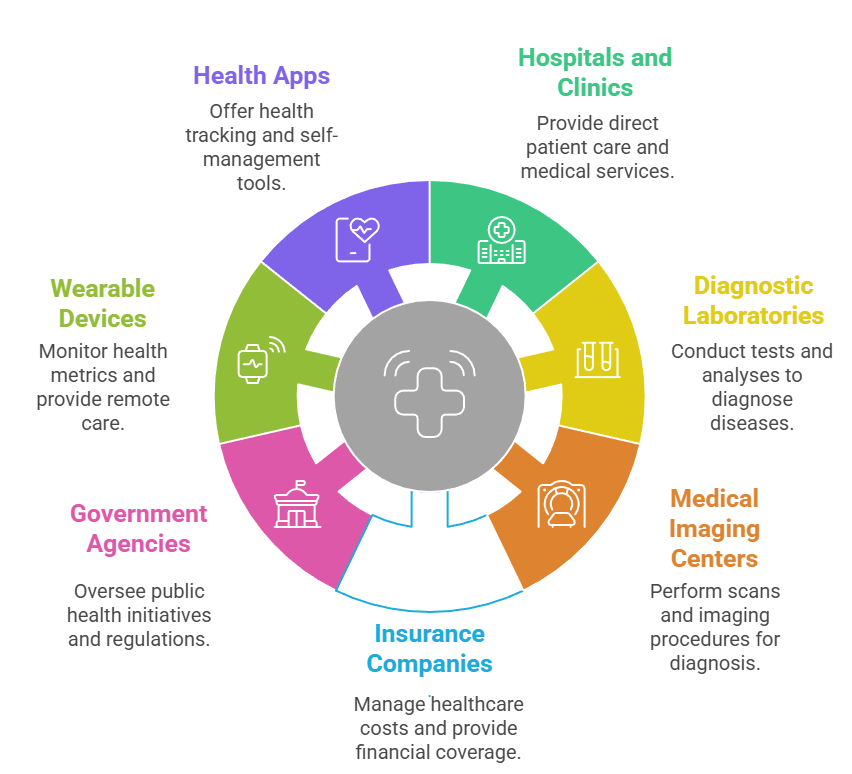
1. Hospitals, Clinics, and Healthcare Providers
Hospitals and clinics are the primary generators of healthcare data through patient interactions, treatments, diagnostics, and routine check-ups. They capture clinical notes, vital signs, imaging studies, lab results, prescriptions, and hospital stay records.
These facilities use EHR systems that centralize patient information and ensure continuity of care. Because hospitals see large, diverse patient populations, the data collected is highly valuable for analytics.
Provider-based data supports predictive modeling, operational planning, quality improvement, and clinical research. It remains the most directand reliable source of patient-specific data.
2. Diagnostic Laboratories and Pathology Centers
Labs generate data from blood tests, biopsies, cultures, hormone panels, viral tests, and metabolic screenings. Their data is structured, standardized, and scientifically validated, making it crucial for accurate diagnosis.
3. Medical Imaging Centers and Radiology Departments
Imaging centers produce diagnostic images such as X-rays, MRIs, CT, and ultrasound scans.
These images are stored in PACS systems, enabling quick access across departments. Imaging data assists in identifying tumors, fractures, organ dysfunctions, and internal structural issues.
Laboratory information systems (LIS) store and transmit test results directly to healthcare providers or EHR systems. Lab data helps clinicians detect disease at early stages and evaluate treatment effectiveness.
Pathology centers contribute critical microscopic and molecular insights that complement clinical evaluations. These facilities serve as a key source for longitudinal and biomarker-based analytics.
AI now enhances the interpretation of such data, reducing radiologist workloads and improving accuracy. Imaging centers also generate metadata like scan type, imaging parameters, and reporting notes.
These sources are vital for building advanced deep learning models in healthcare.
4. Insurance Companies and Healthcare Payers
Insurance organizations generate administrative and claims data during the reimbursement and billing processes. They track patient service use, procedure payments, diagnosis codes, medication claims, and provider details.
This data helps uncover trends in healthcare spending, fraud detection, and cost optimization. Payers also maintain large datasets covering long time periods, making them ideal for population analytics.
Such data reveals patient behavior patterns, chronic disease costs, and treatment utilization. Insurance-based data is crucial for health policy, actuarial analysis, and economic modeling.
5. Government Agencies and Public Health Departments
Agencies such as WHO, CDC, local health ministries, and national health registries produce large-scale public health datasets. These include vaccination reports, disease outbreak statistics, environmental health data, and demographic health indicators.
Governments also maintain national registries for cancer, births, deaths, and infectious diseases.
This data helps track health trends, evaluate public health programs, and guide policymaking. Public health departments serve as authoritative sources because they collect standardized, population-wide data.
These datasets support epidemic prediction, health economics, and healthcare planning.
6. Wearables, IoT Devices, and Remote Monitoring Tools
Wearable devices and IoT health sensors continuously generate physiological and behavioral data outside clinical settings. They capture daily patterns such as heart rate, sleep cycles, physical activity, oxygen levels, and glucose readings.
Remote health monitors allow clinicians to track chronic conditions without frequent hospital visits.
Data from these devices helps detect early health risks and supports personalized treatment plans.
These sources are essential for home-based care models, telemedicine, and preventive healthcare. They also produce real-time data streams required for time-series modeling.
7. Health Apps, Patient Portals, and Self-Reported Tools
Mobile health apps and patient portals allow individuals to record symptoms, medication habits, diet, exercise, and lifestyle patterns. Patient-generated data complements clinical data by providing insights into real-life behavior outside hospitals.
These sources help track chronic diseases, improve medication adherence, and support mental health monitoring.
Self-reported tools offer qualitative information that clinicians may otherwise miss. With rising digital adoption, such apps are becoming a major contributor to healthcare datasets. They empower patients while expanding the scope of available health information.
Types vs Sources of Healthcare Data