Healthcare data standards are structured frameworks that define how health information is collected, stored, exchanged, and interpreted across healthcare systems.
With hospitals, laboratories, insurance providers, and public health agencies relying on diverse technologies, data standards ensure that information flows accurately and consistently between these entities.
Without standardized formats, interoperability breaks down, leading to errors, duplicate tests, delays in treatment, and gaps in patient care.
Modern healthcare increasingly depends on digital systems such as Electronic Health Records (EHRs), telemedicine platforms, and mobile health apps, making standardized communication essential for quality care.
These standards include coding systems for diagnoses and procedures, messaging formats for data exchange, and structural frameworks that dictate how clinical information is organized.
Global standards such as HL7, FHIR, ICD-10, SNOMED CT, and LOINC are widely used to maintain consistency in medical terminology, laboratory results, imaging data, and clinical documents.
Healthcare data standards also ensure compliance with regulatory requirements, patient privacy laws, and clinical safety guidelines.
As healthcare becomes increasingly data-driven, standards support AI and analytics applications by providing clean, structured, and interoperable datasets that can be reliably used for modeling and insights.
Overall, healthcare data standards are essential for interoperability, patient safety, efficient operations, and the scalability of digital health innovations.
Standards and Interoperability in Digital Healthcare Systems
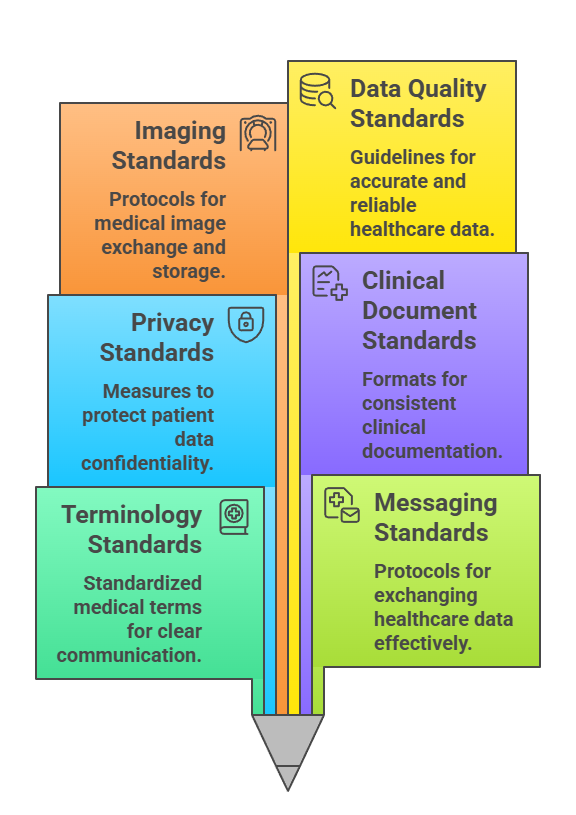
1. Interoperability and the Role of Standards
Interoperability is the ability of healthcare systems to exchange and use patient information seamlessly across platforms, and data standards play a central role in enabling this.
Without standardized terminology, file formats, and messaging systems, hospitals and clinics would not be able to share patient details, causing delays and inconsistencies in care.
Standards such as HL7 and FHIR ensure that clinical systems can communicate even if they use different technologies or vendors.
This reduces medical errors, prevents duplicate testing, and enhances care coordination, especially during emergencies or multi-specialty treatments. Interoperability also improves efficiency by eliminating manual data entry and reducing administrative burden.
With growing use of telehealth and cross-institution data sharing, interoperability standards have become even more essential. They form the foundation of unified, patient-centered healthcare delivery.
2. Terminology Standards (ICD-10, SNOMED CT, LOINC)
Terminology standards ensure that all healthcare providers use consistent and universally understood medical language. ICD-10 provides codes for diseases and health conditions, enabling uniform documentation and billing.
SNOMED CT offers a more detailed, clinically rich vocabulary that supports AI-driven decision systems, EHR interoperability, and advanced analytics.
LOINC standardizes laboratory and diagnostic observations, ensuring that lab results from different labs or devices remain comparable and interoperable.
These standards reduce ambiguity, enhance clinical accuracy, and support meaningful use of data for research and public health. They are crucial for large-scale data aggregation, epidemiological studies, and outcome tracking.
By ensuring uniform terminology, these standards allow healthcare organizations to interpret data consistently and reliably.
3. Messaging and Data Exchange Standards (HL7, FHIR)
Messaging standards such as HL7 and FHIR define how healthcare information is transmitted between systems, enabling secure and structured communication.
HL7 v2 is widely used in hospitals for exchanging lab reports, admission details, and pharmacy data, while HL7 v3 provides more formal specifications for complex workflows.
FHIR, the modern standard, uses web technologies like REST APIs and JSON, making it lightweight, faster, and easier to integrate into mobile apps, cloud systems, and digital health platforms.
These standards enable real-time data sharing across EHRs, wearables, telemedicine platforms, and health information exchanges. They also support patient access to their own health data through apps and portals.
By standardizing exchange formats, messaging standards eliminate fragmentation and enhance the continuity of care.
4. Privacy, Security, and Compliance Standards
Healthcare data standards also address privacy, protection, and regulatory compliance to safeguard sensitive patient information.
Frameworks like HIPAA (U.S.), GDPR (Europe), and DISHA (India – proposed) define how organizations must handle, store, and share health data ethically and securely.
These standards ensure that hospitals implement encryption, access control, audit logs, and consent-based sharing policies. Compliance standards also regulate how long data must be retained, how breaches must be reported, and what penalties apply for violations.
They build public trust by ensuring that patient data is not misused or accessed without authorization.
As cybersecurity threats grow, adherence to privacy and security standards is essential for maintaining safe and reliable healthcare systems.
5. Clinical Document Standards (CDA, CCD, CCR)
Clinical document standards ensure that patient health information is shared in a structured and readable format across different clinical systems. CDA (Clinical Document Architecture) created by HL7 provides a standardized structure for documents like discharge summaries, progress reports, and referral letters.
CCD (Continuity of Care Document) and CCR (Continuity of Care Record) allow essential patient data such as allergies, medications, lab results, and care plans to be exchanged seamlessly between care providers.
These standards ensure that clinicians receive clear, consistent summaries, reducing ambiguity and supporting faster decision-making. They help eliminate redundant data entry and improve the accuracy of care transitions.
With increasing collaboration among specialists and remote care providers, clinical document standards are essential for communication continuity and treatment quality.
6. Imaging Standards (DICOM)
Medical imaging requires specialized data formats, and DICOM (Digital Imaging and Communications in Medicine) is the global standard for storing and transmitting radiology images such as X-rays, MRIs,
CT scans, and ultrasounds. DICOM ensures that both images and related metadata (patient details, scan parameters, interpretations) are preserved in a consistent, interoperable format.
This allows radiologists, surgeons, and AI-based imaging tools to analyze and share images without compatibility issues.
DICOM also supports secure transmission across PACS (Picture Archiving and Communication Systems) to clinics, emergency rooms, and specialists worldwide.
With AI-driven imaging diagnostics growing rapidly, standardized imaging data is essential for model training and clinical validation. Without DICOM, modern medical imaging workflows would be fragmented, error-prone, and difficult to scale.
7. Data Quality Standards (Accuracy, Completeness, Consistency)
Healthcare data quality standards define the criteria required to ensure that clinical information is accurate, complete, consistent, and fit for decision-making.
These standards guide organizations in establishing validation rules, structured entry processes, automated error detection, and quality auditing mechanisms.
High-quality data reduces the risk of clinical mistakes, supports reliable AI models, and enhances patient safety.
Quality frameworks also address issues like missing values, duplicate entries, outdated records, and incorrect coding problems commonly seen in healthcare databases.
By adhering to quality standards, healthcare institutions can produce cleaner datasets for analytics, research, and public health reporting. Ultimately, strong data quality governance ensures that healthcare data remains trustworthy and actionable.
8. Interoperability Frameworks and National Health Information Networks
Many countries have created national digital health frameworks to enforce interoperability standards across all healthcare entities.
Examples include the U.S. ONC Interoperability Standards, India’s ABDM (Ayushman Bharat Digital Mission), and Europe’s eHealth Interoperability Framework.
These frameworks ensure that hospitals, pharmacies, clinics, insurance providers, and government agencies use unified standards for patient identification, data exchange, and EHR formats.
National networks support longitudinal patient records, enabling healthcare providers to view a patient's lifetime health history instantly.
They reduce fragmentation, improve nationwide health reporting, and support large-scale medical research. Such frameworks are becoming essential as healthcare moves toward integrated, nation-wide digital ecosystems.
9. Standards for AI and Machine Learning in Healthcare
As AI becomes increasingly common in diagnostics, treatment planning, and patient monitoring, data standards for AI are emerging to ensure safety, fairness, and explainability.
These standards guide how datasets should be labeled, validated, and documented to avoid bias and ensure transparency.
They also define interoperability between AI models and clinical systems, ensuring that outputs can be integrated into EHRs or clinical workflows.
Standards groups such as ISO and IEEE are developing guidelines for testing AI systems, validating model accuracy, and ensuring ethical use.
These frameworks help healthcare organizations adopt AI confidently without compromising patient safety. By establishing consistency in AI development, these standards accelerate innovation while protecting clinical integrity.
Challenges of Healthcare Data Standards
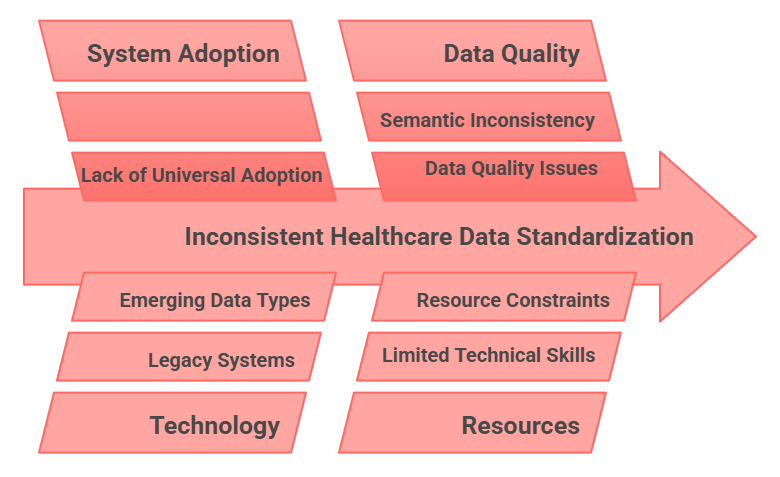
1. Lack of Universal Adoption Across Healthcare Systems
One of the biggest challenges in healthcare data standards is that no single standard is universally adopted across all hospitals, clinics, laboratories, pharmacies, and insurance networks.
Even widely accepted frameworks like HL7, FHIR, ICD, LOINC, or SNOMED CT are implemented differently across organizations.
Some use older HL7 v2 messages, while others partially adopt FHIR APIs but still rely heavily on custom extensions. This creates a fragmented ecosystem where each system speaks a slightly different “dialect,” making seamless data exchange extremely difficult.
As a result, healthcare providers spend significant time building custom interfaces, mapping fields manually, and resolving inconsistencies that arise due to partial or outdated standard implementations.
2. Interoperability Issues Due to Heterogeneous Vendor Systems
Healthcare environments consist of many IT systems built by different vendors—EHR platforms, lab systems, imaging systems, pharmacy systems, billing software, and more.
Each vendor designs their system with proprietary features, making it difficult to enforce standardized data formats.
Even when standards like HL7 or FHIR are technically supported, vendors often implement optional elements differently, or create their own custom fields to meet client-specific needs.
These variations result in interoperability challenges where systems cannot directly communicate without translation layers.
This heavily restricts the true mobility of patient data and increases the risk of misinterpretation or data loss during transfers.
3. Legacy Systems and Limited Support for Modern Standards
Many healthcare organizations still rely on legacy systems developed decades ago, which were not designed for modern metadata structures, standardized vocabularies, or API-based integration.
Upgrading or replacing these systems is extremely costly and risky, as downtime can directly affect patient care. Because of this, healthcare institutions often continue using old systems with minimal modifications.
These systems may not support emerging standards like FHIR, leading to wide gaps in interoperability.
Maintaining compatibility between old and new systems forces organizations to create complex middleware layers, increasing long-term technical debt and operational complexity.
4. Semantic Inconsistency and Varying Clinical Definitions
Standardizing healthcare terminology is deeply challenging because clinical concepts often carry nuanced meanings that depend on context, specialty, location, and clinical workflow.
For example, the term “hypertension” may be coded differently based on severity, stage, or measurement protocol. Local terminologies developed by hospitals may not have direct equivalents in international vocabularies like SNOMED CT.
This semantic inconsistency causes major challenges in analytics, reporting, and interoperability because identical clinical events may be recorded in non-identical ways.
Ensuring semantic clarity requires constant mapping efforts, clinical validation, and frequent updates, which demand time, expertise, and resource investment.
5. Data Quality Issues Affect Standard Compliance
Healthcare data is often incomplete, duplicated, or inconsistently documented due to the pressures clinicians face during patient care. When the source data is poor, even the best standards cannot ensure accurate representation.
For instance, free-text notes may contain essential clinical details that do not map cleanly to structured fields, leaving gaps in standardized datasets.
In lab systems, units may vary between providers, making uniform coding difficult. These quality issues undermine the reliability of data even when standards are technically applied.
As a result, healthcare organizations must invest heavily in validation, cleansing, and normalization processes to maintain usable, standardized datasets.
6. Frequent Updates to Standards and Versioning Problems
Healthcare data standards are not static they evolve continuously. ICD updates disease classifications annually, lab tests get new LOINC codes, and FHIR releases new versions and implementation guides frequently. Keeping all systems aligned with the latest versions is a massive challenge.
Version mismatches between systems can lead to incorrect mappings, incomplete exchanges, or even clinical misinterpretations.
Managing multiple versions of a standard across interconnected hospitals, labs, and pharmacies adds enormous complexity and requires rigorous governance frameworks that many institutions struggle to maintain.
7. Privacy, Consent, and Regulatory Compliance Constraints
Healthcare data sharing must comply with strict privacy laws, patient consent rules, and security requirements.
Standards must support encryption, access controls, audit trails, and consent tracking all while ensuring interoperability. Balancing data access with privacy is particularly difficult when multiple institutions share data.
For example, a FHIR API may expose patient demographics through standardized endpoints, but sharing this data across networks may require explicit patient consent.
Many standards do not inherently handle granular consent rules, forcing organizations to build additional layers of governance, which increases implementation complexity and legal responsibility.
8. Integration of Emerging Data Types (Genomic, Wearables, IoT)
Traditional standards like HL7 and ICD were not originally designed to handle high-dimensional modern data, such as genomics, medical imaging annotations, wearable device streams, or remote monitoring data.
Integrating these emerging data types into existing standards requires new schemas, metadata formats, and interoperability structures.
Genomic data, for instance, produces millions of variants per patient, which cannot be stored using classical EHR coding systems.
Similarly, continuous wearable data generates massive time-series streams that often lack standard definitions. Extending standards to support these data types is ongoing but remains incomplete, creating gaps in analytics and clinical decision-making.
9. Limited Technical Skills and Resource Constraints
Implementing healthcare data standards requires specialized knowledge in clinical informatics, data engineering, vocabulary mapping, and interoperability frameworks.
Many healthcare organizations especially smaller clinics and rural hospitals lack the skilled workforce needed to implement and maintain standards-based systems.
They also face budget constraints that make large-scale infrastructure modernization difficult.
Without adequate skills and resources, organizations often implement standards incorrectly or incompletely, which leads to long-term interoperability problems and increased technical debt.
Class Sessions
Sales Campaign

We have a sales campaign on our promoted courses and products. You can purchase 1 products at a discounted price up to 15% discount.
