Healthcare analytics refers to the systematic use of data, statistical methods, machine learning, and predictive models to generate insights that improve patient outcomes, optimize clinical workflows, and support evidence-based decision-making.
By transforming raw healthcare data into actionable intelligence, analytics enables providers to understand disease patterns, evaluate treatment effectiveness, and improve operational performance.
From early disease detection to real-time monitoring and personalized treatment planning, healthcare analytics plays a critical role in modernizing health systems.
Key concepts in healthcare analytics include descriptive analytics that help summarize past trends, predictive analytics that forecast future risks or events, and prescriptive analytics that recommend best actions to improve outcomes.
Machine learning models, clinical decision support systems, risk stratification tools, and population health dashboards are all central components of today’s data-driven healthcare environment.
These tools help clinicians anticipate complications, prevent hospital readmissions, and allocate resources more efficiently.
Despite its benefits, healthcare analytics faces several challenges rooted in data quality, fragmentation, privacy regulations, and technical limitations.
Healthcare data is often unstructured, incomplete, and stored across isolated systems, making integration difficult. Ensuring patient data privacy under laws like HIPAA and GDPR adds further complexity.
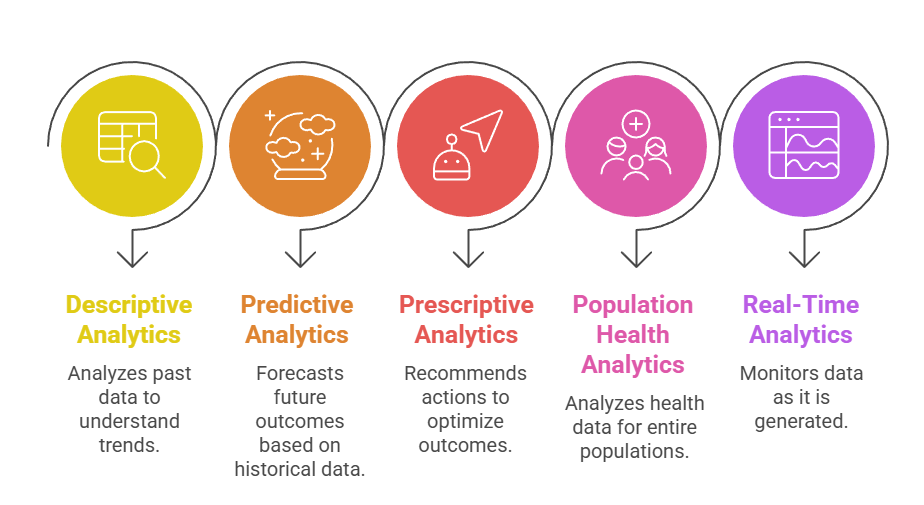
Key Concepts in Healthcare Analytics
 1. Descriptive Analytics
1. Descriptive Analytics
Descriptive analytics focuses on summarizing historical healthcare data to understand trends, patterns, and overall performance. It helps providers analyze past admissions, treatment outcomes, medication use, and operational metrics.
Dashboards and visualization tools highlight key indicators such as mortality rates, infection patterns, and average length of hospital stay. These insights support quality improvement programs by identifying areas that need attention.
Descriptive analytics forms the baseline for advanced analytics by providing a clear picture of what has happened. It enables administrators and clinicians to track progress, compare performance, and evaluate the effectiveness of interventions.
2. Predictive Analytics and Risk Stratification
Predictive analytics uses statistical models and machine learning to forecast future clinical events such as disease progression, readmission risk, or likelihood of complications.
Hospitals use risk stratification tools to categorize patients based on their future health risks, enabling more targeted and proactive care.
Predictive algorithms analyze EHR data, vital signs, lifestyle factors, and lab values to detect early signals of deterioration. This helps clinicians intervene earlier, reducing preventable emergencies.
Predictive analytics also improves resource planning by forecasting patient loads and identifying high-risk populations. Overall, it strengthens preventive care and enhances patient safety.
3. Prescriptive Analytics and Clinical Decision Support
Prescriptive analytics goes beyond predicting outcomes by recommending specific actions that can produce the best clinical results. These models guide treatment selection, dosage optimization, and personalized care pathways.
Clinical Decision Support Systems (CDSS) use prescriptive insights to alert doctors about unsafe medications, drug interactions, or deviations from clinical guidelines.
These tools help standardize care and reduce errors, especially in busy hospital environments.
By integrating patient history, real-time data, and medical knowledge, prescriptive analytics supports precise, evidence-based decision-making. Its value lies in helping clinicians adopt the most effective interventions at the right time.
4. Population Health Analytics
Population health analytics examines health data at the community or population level to identify broader trends, disparities, and risk factors. It helps public health agencies monitor chronic disease prevalence, vaccination coverage, and outbreak patterns.
Hospitals use population analytics to understand social determinants of health, such as income and environment, which influence patient outcomes.
These insights support targeted programs for vulnerable groups and guide policy decisions.
By combining clinical, demographic, and environmental data, population analytics helps reduce inequalities and strengthen public health planning. It is crucial for preventive care and large-scale health improvement.
5. Real-Time Analytics and Remote Monitoring
Real-time analytics involves processing current patient data from EHR systems, wearables, or bedside monitors to enable immediate clinical decisions. It plays a key role in emergency care, ICU monitoring, and early-warning systems for sepsis or cardiac arrest.
Wearables and IoT devices continuously stream data, giving clinicians a complete view of patient status outside hospitals. Real-time insights reduce delays, support timely intervention, and improve outcomes for high-risk patients.
This capability is essential for telemedicine, virtual care, and home-based chronic disease management. Real-time analytics enhances responsiveness and strengthens patient safety.
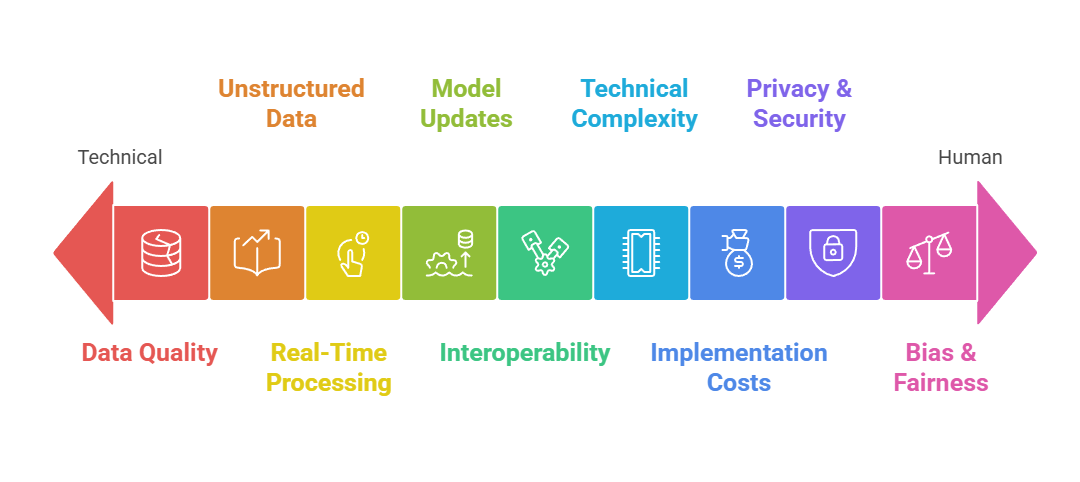
Challenges in Healthcare Analytics
 1. Data Quality, Inconsistency, and Fragmentation
1. Data Quality, Inconsistency, and Fragmentation
Healthcare data often comes from multiple systems—EHRs, labs, imaging, and wearables—which may not follow the same standards. Incomplete, inconsistent, or duplicated data reduces model accuracy and complicates analysis.
Many hospitals still rely partly on manual documentation, increasing the risk of errors.
Fragmented systems hinder interoperability and require extensive data cleaning or integration before analytics can begin.
Poor data quality can lead to incorrect conclusions, unsafe predictions, and reduced trust in analytic tools. Ensuring accurate, standardized data is one of the biggest challenges in healthcare analytics.
2. Privacy, Security, and Ethical Concerns
Healthcare data is highly sensitive, and protecting patient privacy is critical. Regulations like HIPAA and GDPR set strict rules for data access, sharing, and storage.
Analytics teams must ensure encryption, secure access controls, and ethical handling of patient information.
Data breaches can lead to major harm, including identity theft and loss of patient trust.
Ethical concerns also arise when using patient data for secondary purposes like research or AI training.
Healthcare organizations must balance innovation with strict privacy protections to maintain safety and compliance.
3. Bias, Fairness, and Model Interpretability
AI models trained on biased or unrepresentative datasets may produce unfair outcomes, affecting certain demographic groups more than others. This can lead to unequal treatment recommendations or misdiagnosis.
Clinicians also require models to be transparent and interpretable to trust their outputs.
Black-box algorithms create risk if their decision-making cannot be explained. Ensuring fairness, reducing bias, and improving interpretability are essential for safe clinical adoption.
Healthcare analytics must follow ethical guidelines to ensure equitable and trustworthy results.
4. Technical Complexity and Skill Gaps
Implementing healthcare analytics requires expertise in data science, medical knowledge, regulatory compliance, and system integration.
Many healthcare organizations lack trained data professionals or sufficient infrastructure. Integrating AI tools with legacy hospital systems is technically challenging and resource-intensive.
Clinicians may also need training to effectively use data-driven tools.
These skill gaps slow down analytics adoption and reduce the impact of digital initiatives. Addressing these challenges requires investment in training, collaboration, and modern technologies.
5. Interoperability Issues Across Healthcare Systems
Healthcare data is stored across multiple platforms such as EHR systems, imaging servers, lab databases, and pharmacy systems, each using different formats and standards.
Because these systems often cannot communicate easily, integrating data into a unified platform becomes difficult. Lack of interoperability leads to incomplete patient profiles and limits the effectiveness of analytics models.
Hospitals struggle to combine structured, unstructured, and real-time data without major transformation efforts.
This also slows down clinical decision-making when information is scattered across systems. Improving system compatibility is crucial for building accurate analytics workflows and enabling seamless data sharing across departments and organizations.
6. High Implementation Costs and Infrastructure Limitations
Advanced analytics tools require powerful computing systems, cloud storage, secure networks, and specialized software. Many healthcare facilities, especially smaller hospitals or rural centers, lack the financial resources to invest in such infrastructure.
Additionally, maintaining data pipelines, updating systems, and hiring trained professionals adds ongoing costs.
Without proper infrastructure, healthcare organizations cannot process large datasets or deploy machine learning solutions effectively.
This creates inequalities in access to analytics capabilities, limiting innovation in resource-constrained settings. Cost-related barriers remain one of the biggest obstacles to broad adoption of healthcare analytics.
7. Resistance to Change Among Healthcare Professionals
Introducing analytics, AI tools, and automated systems often changes traditional workflows, which some clinicians may view with skepticism.
Healthcare professionals may fear that analytics tools will replace their expertise or introduce extra work during documentation.
Lack of familiarity with data-driven systems can also reduce trust in algorithmic recommendations.
This resistance slows down adoption and reduces the effectiveness of new technologies.
Training, communication, and demonstrating the practical benefits of analytics are essential to overcome these cultural barriers. Acceptance from clinicians is crucial for integrating analytics into routine care.
8. Real-Time Data Processing Challenges
Real-time analytics depends on continuous data streaming from monitors, wearables, and EHR systems.
Handling these high-velocity data streams is technically complex, requiring low-latency processing and immediate response capabilities. Interruptions in connectivity, sensor failures, or system delays can affect data accuracy.
Hospitals must maintain reliable networks and monitoring systems to ensure uninterrupted data flow.
Real-time systems also require robust alert mechanisms that do not overwhelm clinicians with unnecessary notifications. Ensuring stable, reliable real-time analytics remains a significant technical challenge.
9. Unstructured Data and Difficulties in Text Processing
A large portion of healthcare data—doctor notes, discharge summaries, imaging reports, and patient feedback—is unstructured.
Processing such data using NLP techniques is challenging because clinical language includes abbreviations, variations, and context-dependent meanings. Misinterpretation of unstructured data can lead to inaccurate insights or faulty predictions.
Converting unstructured data into usable formats requires advanced AI models and careful validation.
This adds significant complexity to healthcare analytics workflows. Improving unstructured data processing is crucial for achieving comprehensive and accurate analytics results.
10. Constant Need for Model Updates and Monitoring
Healthcare is dynamic, with new diseases, updated clinical guidelines, and evolving population health patterns. Analytics models can quickly become outdated if they are not regularly updated with new data.
Outdated models may produce inaccurate predictions, reducing trust among clinicians. Continuous monitoring, retraining, and validation of models require time, expertise, and computational resources.
This ongoing maintenance is often overlooked during initial implementation. Without systematic model governance, healthcare analytics systems cannot remain reliable or clinically effective.
11. Legal and Regulatory Compliance Challenges
Healthcare organizations must comply with regulations such as HIPAA, GDPR, and various national health data protection laws. Ensuring that analytics projects meet all compliance requirements often involves complex auditing, documentation, and legal review.
Sharing data across institutions—such as for research or AI training—can raise legal concerns about consent and data ownership. Non-compliance can lead to severe penalties and reputational damage.
These legal complexities slow down innovation and limit the scope of data-sharing initiatives. Navigating regulations effectively is essential for safe and lawful analytics use.
